A Patient’s Guide to Reverse Total Shoulder Replacement (Reverse Shoulder)
Introduction
Yearly, there are approximately 50,000 shoulder replacements performed. Last year the number of reverse shoulder replacements (reverse shoulder prosthesis) was higher than the number of standard (anatomic) replacements. Early indications for reverse shoulder replacement were patients with arthritis and rotator cuff tearing (rotator cuff arthropathy). These indications have expanded to include massive rotator cuff tears with poor function (pseudo paralysis), 3 and 4 part proximal humerus fractures in older individuals, and revision surgery for partial or total replacement. Dr. Groh is the chief designer of the shoulder replacement you will receive for this condition.
Anatomy
The shoulder serves as a connection between the chest and arm. The clavicle functions as a strut connected to the shoulder bone (scapula). The scapula articulates with the humerus and accounts for approximately 70% of shoulder motion (the remaining motion occurs between the scapula and the thorax). Your shoulder is made up of three bones: your upper arm bone (humerus), your shoulder blade (scapula), and your collarbone (clavicle).
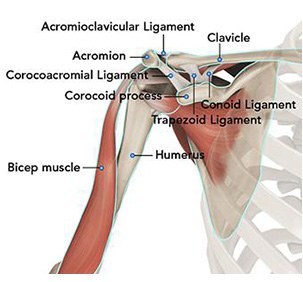
A right shoulder viewed from the front showing the clavicle, humerus and scapula.
The motion between the shoulder blade and scapula is a stable gliding surface over bursal structures and not prone to dislocation. However, the articulation between the humerus and scapula has little bony stability. This is because the ball of the humerus is large and the socket is small on the scapular side—think of the small amount of stability a golf ball has on a tee.
The inside layer of muscles gives the shoulder stability and motion above shoulder height and is called the rotator cuff—a series of 4 muscles
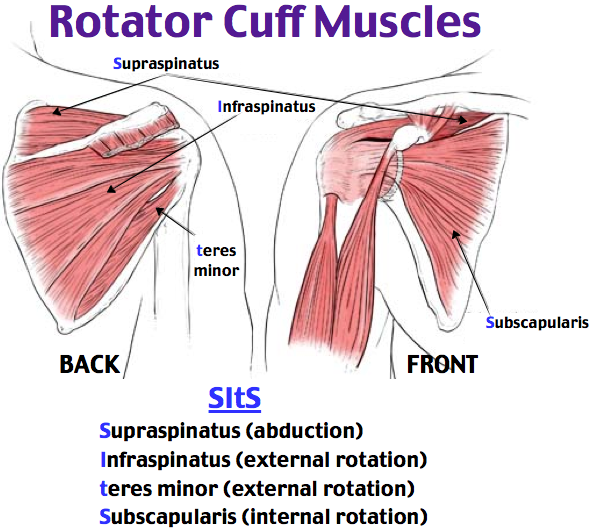
The muscles underlying the deltoid—the rotator cuff viewed from the back and front
Because of the necessity for the rotator cuff to stabilize the ball of the humerus, an anatomic or standard shoulder replacement is not indicated for patients with an incompetent rotator cuff. In these situations, a different type of replacement called a reverse shoulder replacement is indicated. A reverse shoulder replacement restores stability to the shoulder, allows for increased shoulder motion, and relieves pain.
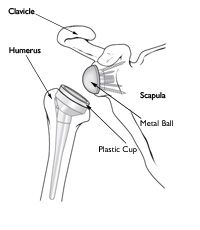
A diagram of a reverse shoulder replacement—the plastic cup replaces the ball of the humerus. A metal ball replaces the shallow socket of the scapula (shoulder blade)
Diagnosis
Symptoms
Patients report pain and inability to raise the arm with rotator cuff arthropathy (arthritis and massive tearing of the rotator cuff). This greatly limits the function of these patients—many are unable to get a glass from a shelf, comb their hair or reach across the table to grab the salt shaker. Pain may be worse at night and interfere with sleeping.
Surgeon Examination
After reviewing the patient’s symptoms, a review of their pertinent medical history and family history is obtained. The range of motion of the shoulder is measured in multiple planes. The strength of the shoulder in resisting motions is tested.
Imaging
X-rays can determine the amount of arthritis associated with the disease. Typically x-rays from multiple angles better discern the amount of arthritis. Patients with chronic rotator cuff tearing may exhibit changes in relationship of the ball and socket which indicates a massive chronic tear with a high riding humeral head.
Enhanced imaging of CT or MRI may be used to further image bone for reconstruction. MRI may be used to evaluate the status of the rotator cuff when it is unclear regarding the rotator cuff integrity.
Treatment
Nonoperative
Many patients with massive rotator cuff tears may respond to nonoperative treatment. The typical course is to inject the shoulder with steroid and enroll the patient in a formal physical therapy program with emphasis on strength of the anterior glenoid. Dr. Groh reported his results with this program and followed patients for approximately 5 years. 70% of patients treated with this technique did not require surgery and their results were stable over the length of follow up.
Operative
For patients with continued pain and poor function, reverse shoulder arthroplasty is an excellent option. Results are shown in all studies to correlate with surgeons who do a considerable volume of shoulder replacement every year. The average orthopedic surgeon performs less than five shoulder replacements per year. Dr. Groh performs over 175 shoulder replacements in an average year.
The anesthesia choices include regional or general anesthesia. Incisions are required to place hardware for the reverse procedure into position. Dissection to identify nerves and bone landmarks usually makes for an exacting procedure—requiring a subspecialist.
Dr. Groh performs over 90% of shoulder replacement surgery as an outpatient. Surgery is typically performed with a nerve block and supplemental anesthesia. Surgery typically requires less than 90 minutes, and the risks of blood transfusion are 1% in most studies.
The length of incision for a typical shoulder replacement is two inches in females and three inches in muscular males. Dr. Groh utilizes negative pressure wound management systems to improve wound healing and decrease the risk of infection. Patients may shower as desired with this wound management system and do not need to change dressings at home.
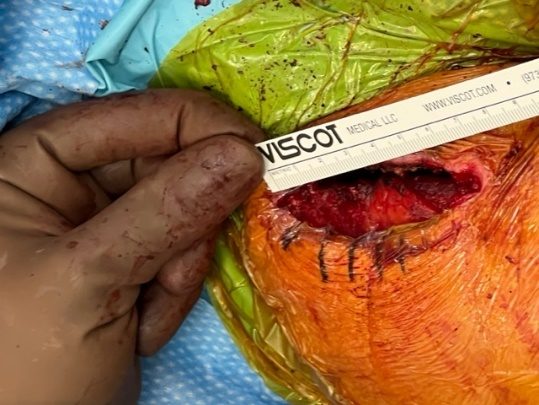
Postoperative incision prior to closure for shoulder replacement in a muscular male—measuring seven centimeters (just under three inches)
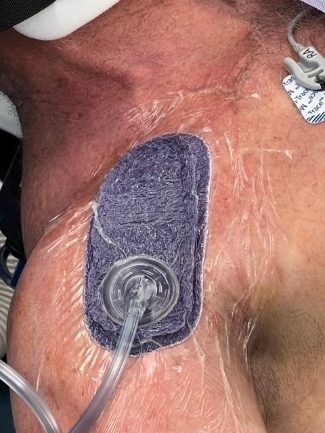
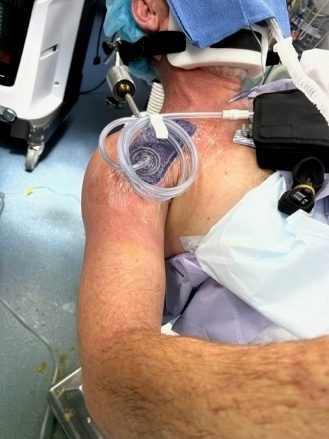
Negative pressure wound management system in place at the conclusion of shoulder replacement. The surgical incision is approximately half the size of the purple wound management sponge.
WATCH AN ANIMATION VIDEO OF REVERSE SHOULDER REPLACEMENT
WATCH A VIDEO OF REVERSE SHOULDER REPLACEMENT FOR SHOULDER FRACTURE
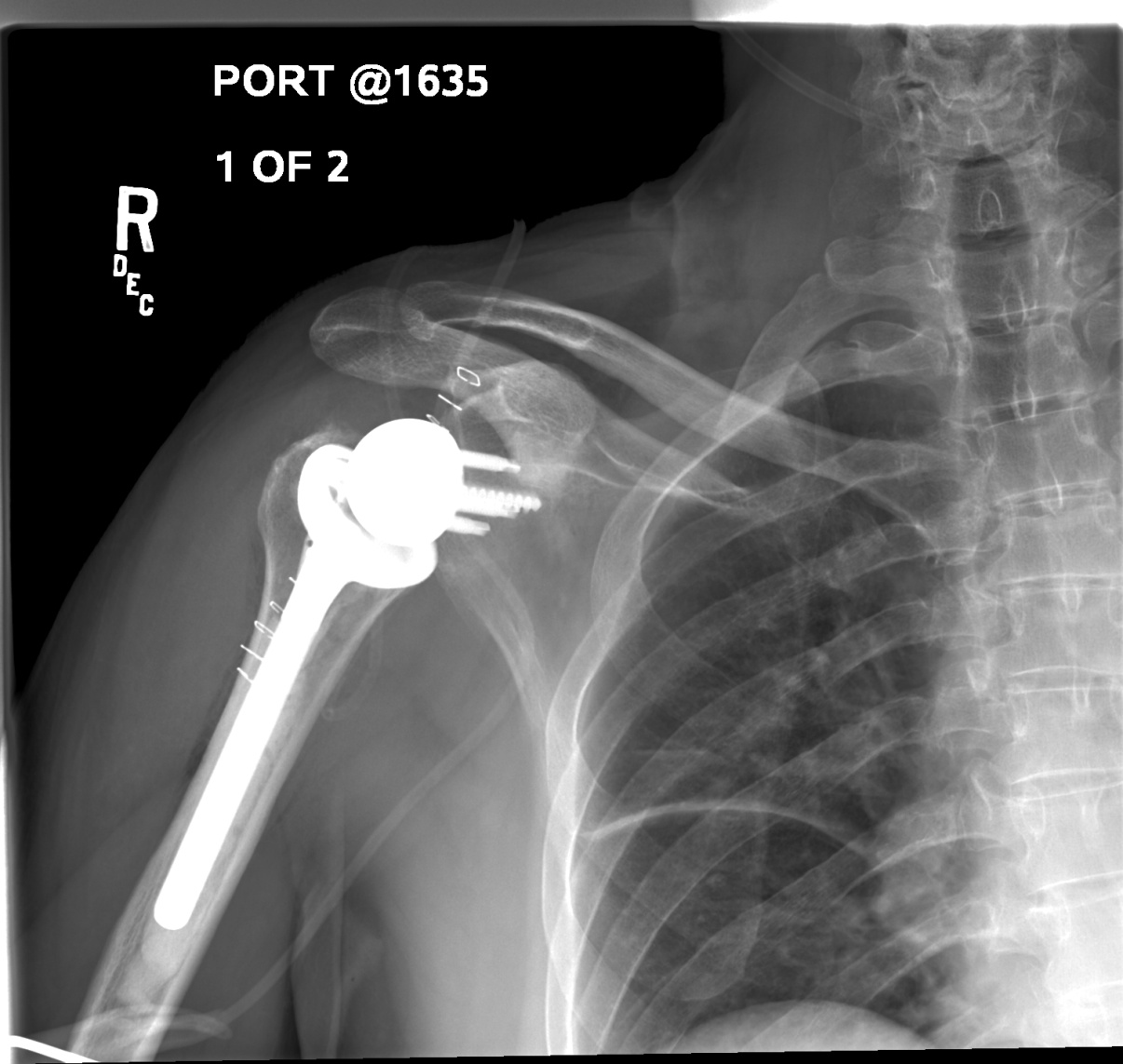
A postoperative x-ray of right reverse total shoulder viewed from the front
Rehabilitation
After surgery the arm is immobilized in a sling to allow for wound healing. Patients report pain after surgery, but the pain generally improves after the first day and utilization of multimodal pain techniques have been shown to improve outcomes for patients. Most patients will report resolution of their preoperative deep achy pain within the first two weeks and note their pain from the surgery has subsided considerably.
Many studies have shown that patients can successfully rehabilitate their shoulder on their own at home. Patients are typically guided through a therapy program and weaned from their sling over the first 2 months. Ingrowth of the components typically requires 3-4 months and patients may return to golf by 4 months after surgery. Continued work on motion and strength allows form improvement for up to 1 year after surgery.
Dr. Groh is an expert shoulder replacement surgeon.
- Named top 60 Shoulder Surgeon in the USA by Becker’s Orthopedics
- Active member of the American Shoulder and Elbow Surgeons
- Written 50 Articles and Textbooks on Shoulder Injuries
- Holds patents and developed multiple shoulder implants and devices including reverse shoulder replacement and standard shoulder replacement


